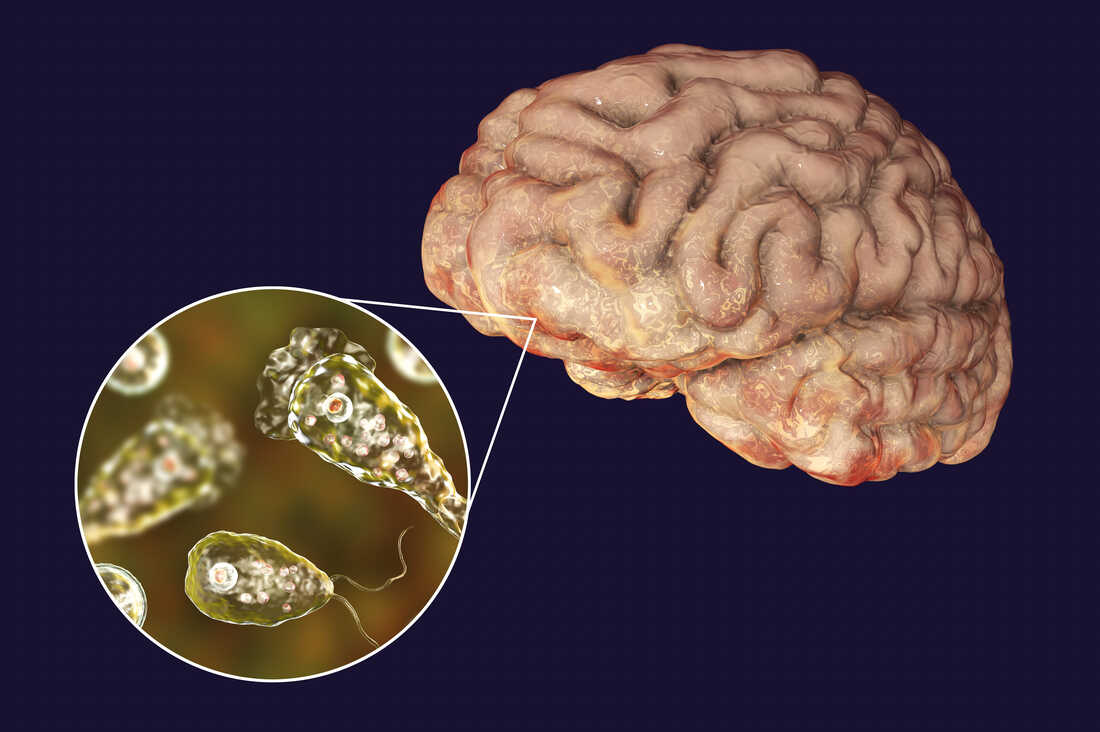
Introduction to Naegleria fowleri
The “brain-eating amoeba” or Naegleria fowleri is a species of the genus Naegleria. It is not a real amoeba, but rather a shape-shifting amoebo flagellate excavate.it is a member of the phylum Percolozoa. The major food source of this free-living creature brain-eating Amoeba is bacteria, but it has the potential to turn pathogenic and cause naegleriasis, also known as primary amoebic meningoencephalitis (PAM). It is a very uncommon, severe, and typically fatal brain illness.
This brain-eating Amoeba is Typically present in warm freshwater bodies of water, including ponds, lakes, rivers, hot springs. And also in industrial or power plant warm water discharge, geothermal well water, swimming pools with low levels of chlorine (less than 0.5 mg/m3), water heaters, soil, and pipes carrying tap water. Either an amoeboid stage or a transient flagellate stage is possible.
The pathogen was given the name Malcolm Fowler after the first person to publish the PAM case reports. An Australian pathologist at Adelaide Children’s Hospital. The first person to write the initial series of case reports for PAM was an Australian pathologist at Adelaide Children’s Hospital named Malcolm Fowler, after whom the organism was named.
The thermophilic, free-living brain-eating amoeba Naegleria fowleri is typically present in warm, hot freshwater areas like ponds, lakes.. Its population tends to grow as temperatures rise. The amoeba is thought to have developed in the United States. Even though it was first discovered in Australia in the 1960s. There are three different types of N. fowleri: cyst, trophozoite (ameboid), and biflagellate. The flagellate form has been present in cerebral fluid. However it does not produce cysts in solid human tissue, which only possesses the amoeboid trophozoite stage.
Life Cycle and Habitat
Trophozoites change into microbial cysts in order to withstand extreme environmental conditions. The cyst is a single-layered, spherical structure with a diameter of 7 to 15 m that surrounds the nucleus of a single cell. The cyst serves as a tough casing that enables the amoeba to tolerate challenging conditions. Lack of food, crowding, desiccation, waste buildup, and freezing temperatures are factors that cause cyst formation. When the situation gets better, the amoeba can come out of the cyst’s central pore or ostiole. It is note that N. fowleri encysts at temperatures lower than 10 °C (50 °F).
For humans, the infectious stage is the trophozoite stage, during which the organism can actively feed and proliferate. The trophozoite adheres to the olfactory epithelium before travelling through the cribriform plate in the nasal cavity and into the brain along the axons of olfactory receptor neurons. The protozoan organism’s reproductive stage transforms at around 25 °C (77 °F). And thrives best at about 42 °C (108 °F), where it multiplies via binary fission.
Trophozoite Characteristics and Behavior
Trophozoites identify by the flexible membrane that surrounds their nucleus. They stretch and fill pseudopodia, or extensions of their cell membrane, with protoplasm to move. Pseudopods grow in the direction of the motion. When trophozoites are free-living, they consume bacteria. They appear to phagocytize (enclose and digest) red blood cells in tissues and cause tissue damage either by releasing cytolytic chemicals or by coming into direct contact with neighbouring cells while using cytolytic membrane proteins.
On their membrane, Naegleria fowleri trophozoites form one to twelve amoebastomes (amorphous cytostomes), which are frequently referre to as “suckers” or “food cups,” and which they use for feeding in a way analogous to trogocytosis.
Naegleria fowleri is biflagellate, or having two flagella, and has a pear-shaped flagellate stage. When diving or swimming, for instance, this stage might be inhale into the nasal cavity. When trophozoites are place in distilled water, for example, they are subject to a change in the ionic strength of the fluid. They are in, which results in the flagellate form. Although the flagellate form is absent from human tissue, it is found in cerebrospinal fluid. A trophozoite emerges from the flagellated form once it has entered the nasal cavity. Within a few hours, this transition takes place.
Environmental Factors
Excavata Naegleria fowleri lives in water and soil. It cannot thrive in seawater since it is sensitive to acidic and drying environments. Since the amoeba flourishes at somewhat high temperatures, summertime is when infections are most likely to occur. As a facultative thermophile, N. fowleri may thrive at temperatures as high as 46 °C (115 °F). Amoebae can live in warm freshwater when there is a sufficient supply of bacteria for food. Artificial bodies of water, altered natural ecosystems, and sites with soil, unchlorinated water, or unfiltered water are among the places where numerous amoebic infections have happened.
It seems that N. fowleri thrives when there is unrest. According to the “flagellate-empty” hypothesis, the reason Naegleria thrives when thermosensitive protozoal fauna doesn’t is because there is less competition. In other words, N. fowleri flourishes in the absence of other predators who would otherwise deplete its food supply. According to this theory, human interferences such thermal pollution lead to an increase in N. fowleri population by driving out rivals for scarce resources. Amoeboflagellates can disperse more easily in areas devoid of rival species thanks to their motile flagellate stage.
Naegleriasis, commonly known as primary amoebic meningoencephalitis (PAM), amoebic encephalitis/meningitis, or simply Naegleria infection. It is a typically fatal infection of the brain that N. fowleri may cause. Although there have been incidences in cooler climates like Minnesota, US. Infections often happen after swimming in freshwater in a warm environment. In rare instances, nasal or sinus irrigation with contaminated water in a nasal irrigation tool like a neti pot has resulted in illness.
Normally, N. fowleri feeds on bacteria, but when it infects humans, the trophozoites eat astrocytes and neurons. Since Naegleria and Acanthamoeba contain a structural homolog of animal CHRM1. It has been hypothesis that the neurotransmitter acetylcholine may operate as a stimulus that causes N. fowleri to traverse the cribriform plate.
Symptoms, Diagnosis, and Treatment of Naegleriasis
After nasal exposure to N. fowleri flagellates, symptoms take one to nine days (on average five) to manifest. Headache, fever, nausea, vomiting, loss of appetite, changed mental status, coma, drooping eyelid, blurry vision, and taste loss are symptoms that may appear. Later symptoms could include hallucinations, convulsions, confusion, lack of focus, stiff neck, and difficulty of balance.
Animals can be infected with Naegleria fowleri, albeit this is infrequently seen. PAM has been report in cattle and South American tapirs, as well as mice, guinea pigs, sheep, and other experimental animals. Animal illness is probably underappreciated.
The antifungal drug amphotericin B, which inhibits the pathogen by attaching to its cell membrane sterols, causes cell membrane rupture and pathogen death, is the main component of antimicrobial therapy. Nevertheless, even with this therapy, the fatality rate is higher than 95%. There is a need for novel therapies. Miltefosine, an antiparasitic medication, suppresses the pathogen by severing the signal pathway, which it has been utilise in a few cases with varying degrees of success.
The timeliness of diagnosis is a crucial component of successful treatment. Since naegleriasis is uncommon and frequently not thought to be the cause, the clinical laboratory’s identification of the bacterium may be the first time an amoebic aetiology is taken into consideration. Delays in diagnosis and treatment may be avoid with the help of the quick identification. PAM can be diagnose with amoeba cultures and real-time polymerase chain reaction (PCR) tests for N. fowleri, however these tests are not commonly available at most institutions and must be carry out at a reference laboratory.
Diagnostic Challenges
Given that PAM has a varied incubation period that can last anywhere between 1 and 7 days, the patient’s timing of presentation may potentially have an impact on the microorganism’s identification. The clinical symptoms of PAM, such as fever, stiff neck, and severe headaches, are comparable to those of viral and bacterial meningitis. Long-lasting nausea, vomiting, and even seizures might develop from the initial symptoms. Acute hemorrhagic necrotizing meningoencephalitis, which can cause mortality in as little as 7–10 days, can develop from the condition.
The length of time between a patient’s exposure to symptoms. Their arrival for treatment at a medical facility, the workup of the diagnosis (initial diagnosis of likely bacterial meningitis). And finally the time between the diagnosis and the start of recommended therapy can all contribute to a variable delay in treatment. Only after accurate diagnosis, which depends on pathologists and medical technologists quickly identifying the bacterium, can successful treatment of PAM be try. Medical technologists must regularly give early CSF evaluation, consider PAM as a diagnosis, and search for amoebae in cases of meningitis, especially during the summer.